Abstract
Background:
The COVID-19 pandemic has changed the mode of education, causing universities to shift from face-to-face to online delivery mode for offering various courses and programs. Thus, it is essential to focus on the curriculum content to tackle the challenges caused by the COVID-19 pandemic and provide methods to effectively educate nursing students in nursing practice.Objectives:
This study aimed to determine the clinical effectiveness of virtual nursing process (NP) education in undergraduate nursing students during the COVID-19 pandemic.Methods:
This educational evaluation study with a quasi-experimental longitudinal design was applied in four educational steps over six months for first-year undergraduate nursing students (n = 30) using Iran's national learning virtual environment.Results:
The paired t-test results showed a significant difference in the mean and overall scores of nursing diagnosis and nursing outcomes/goals before and after the virtual intervention (P < 0.001). Six months after virtual education, the students registered for the ‘clinical nursing process (CNP) unit in the third semester. In the final step of the study, the overall mean score of the students' nursing care plan was 16.59 ± 2.31, which was higher than the mean score, meaning virtual NP education was effective in a clinical setting.Conclusions:
Virtual mode of teaching can be effective for theoretical and CNP education.Keywords
1. Background
Educational institutions in nursing have always looked for methods to increase educational efficiency and enhance teaching and learning quality. They have emphasized the importance of changing education delivery mode, from redesigning curricula to developing innovative learning applications (1). Virtual education is an effective learning method that provides an environment for acquiring clinical competencies (2). It aims to be more student-oriented and assumes that new knowledge is constructed on previously acquired knowledge (3).
During the COVID-19 pandemic, we have been forced to adapt to new circumstances in all aspects of our lives. Likewise, the field of education has undergone essential changes. The entire educational system from elementary to higher levels has collapsed globally during the lockdown period due to COVID-19 (4). It has constantly changed educational settings, causing universities to shift from face-to-face to online delivery mode for offering various courses and programs (5). Likewise, many in-person classes at Iranian universities were suspended, but instruction has been continued thorugh virtual learning, which is an essential part of the process. In this regard, it is necessary to take several steps, including developing infrastructures and properly training students and teachers to adapt to online teaching (4). Although several studies show that virtual education is an effective method for teaching and learning (3, 6), there are still unfulfilled needs in terms of access to digital resources and socio-emotional needs. Virtual teaching dissatisfied students because of poor internet connectivity, digital equipment delivery, and health problems caused by socio-economic problems, mainly at the beginning of classes (7). In this regard, the Virtual University of Medical Sciences of Iran designed the Navid software for virtual learning, and the Babol University of Medical Sciences, Babol, Iran, made the use of the software compulsory for theoretical courses in a virtual setting. The software is a national learning management system with which instructors share materials and students collaborate, discuss, and manage assignments and quizzes.
Using Navid in teaching the nursing process (NP) theory course led instructors to switch from face-to-face and workshop-style formats to a virtual framework. Although virtual learning is considered a desirable phenomenon and has been increasingly used by higher education institutions before and during the pandemic, there are limited studies on the effectiveness of virtual NP education, and there is, therefore, room for improvement through effective, comprehensive evaluation measures (8), especially in clinical environments. In this regard, the present study aimed to determine the effectiveness of virtual NP education among nursing students of Ramsar Nursing and Midwifery School from May 2020 to Dec 2020.
2. Objectives
The study’s first objective was to determine the effectiveness of virtual education in learning NP. The study’s second objective was to determine the effect of virtual education on applying NP in clinical settings. We hypothesized that virtual NP education would be positively effective in learning NP and applying it in clinical settings.
3. Methods
This educational evaluation study with a quasi-experimental longitudinal design was conducted in four educational steps for 30 first-year undergraduate nursing students using the census sampling method over six months. The study's inclusion criteria for the first three steps were: (1) passing the theoretical and practical the ‘fundamentals of nursing skills’ course; and (2) registering for the ‘NP’ course. The study's exclusion criteria were: (1) failure to provide assignments; and (2) transferring to another university before the final step. Most of the students used the Navid software by installing it on their cell phones.
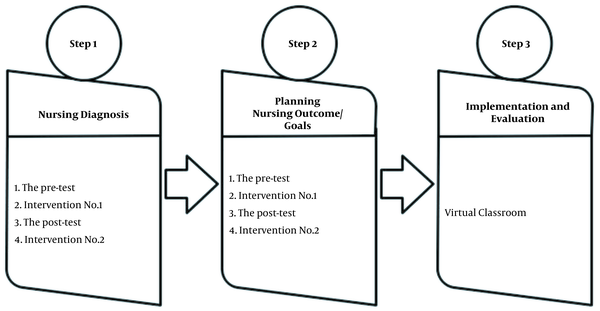
In the fall semester before the pandemic, the assessment phase of NP was instructed face-to-face. However, the instructors were forced to virtually deliver the other four phases in the spring semester due to the pandemic. Head of department approval was obtained prior to study initiation. Although the students were not aware that they were participating in a research, one of the researchers was the course instructor in all of the steps. In the beginning, the students were provided with the virtual course’s objectives, teaching method, and references through Navid, and then the following steps were performed, as depicted in Figure 1.
The virtual education steps
3.1. Step 1. Nursing Diagnosis
This step was performed in four sections.
3.1.1. The Pre-test
An imaginary patient history was uploaded to the system. Before studying any ND reference, the students were tasked to develop all possible ND for the patient and submit their answers to the system in 24 hours.
3.1.2. Intervention
After submission, the researchers translated the latest NANDA list into Persian, and the instructor’s recorded voice with PowerPoint presentations were uploaded to the system. The instructor recordings and presentations contained a review of the NP basics, requirements for this process, descriptions of its stages, other necessary information, and an introduction to the imaginary patient's problems.
3.1.3. The Post-test
The students were asked to write and submit ND based on the NANDA list and what they had been taught about the imaginary patient under the virtual supervision of the instructor in four days. The post-test had 1.5 points.
3.1.4. Intervention No.2
After the post-test, all the students were given feedback and the ability to discuss their opinions on their pages in the system. Finally, the instructor uploaded the corrected ND to the system.
3.2. Step 2. Nursing Outcomes/Goals
This step was performed in four sections.
3.2.1. The Pre-test
Following the previous step, the students wrote possible outcomes/goals for the corrected nursing diagnosis and submitted them to the system 24 hours before studying any NP references.
3.2.2. Intervention
Afterward, the third stage – planning (priorities, nursing outcomes/goals, and nursing interventions) – was introduced by uploading the instructor’s recorded lessons and PowerPoint presentations.
3.2.3. The Post-test
The students were asked to write and submit possible nursing outcomes/goals for the corrected ND to the system in four days under the virtual supervision of the instructor. Due to updating of the Navid software, it was not available for two days, and, therefore, the students were provided with guidance and corrected using WhatsApp.
3.2.4. Intervention
Then, the instructor uploaded the final corrected nursing outcomes/goals to the system. The post-test had 1.5 points.
3.3. Step 3. Implementation and Evaluation
This step was taught using a 60-minute virtual classroom.
3.4. Step 4. Clinical Evaluation
Six months after virtual education, the students registered for the ‘clinical nursing process’ (CNP) unit in the third semester. According to the educational plan, the students were divided into four groups. The educational curriculum was designed for a 9-day internship, and the instructor started the fourth step after obtaining approval from the head of the department.
The inclusion criteria of the step were: (1) passing the ‘fundamentals of nursing skills’ clinical course; (2) passing the ‘NP' course, which is offered virtually; and (3) registering for the CNP course. The exclusion criteria of the step were: (1) being absent for more than one session in the CNP course; and (2) failure to provide NCP for a patient. Three students did not attend the course due to transferring to another university, and another one did not attend the course due to positive COVID-19 test results.
The data was collected based on the NP score checklist approved by the department. Based on the checklist, 5 points for assessment, 5 points for ND, 3 points for nursing outcomes/goals, 7 points for nursing interventions, 5 points for implementation, and 5 points for evaluation were given. The students were asked to prepare an NCP and implement it for patients based on what they learned from the virtual NP education course.
On the first day of the CNP course, each student completed the assessment form, provided the ND based on the latest Persian NANDA list, specified expected nursing goals/outcomes, and presented them in the group. Under the instructor's supervision, the other students discussed and exchanged ideas about ND and nursing goals/outcomes and corrected them if necessary. Then, using nursing references, each student prepared their nursing interventions, presented them to the group, and discussed and corrected them if necessary. The interventions were implemented for the patient and evaluated under the supervision of the instructor.
Due to the COVID-19 pandemic and the shorter-stay policy for non-COVID-19 patients in hospitals, the patients were mostly discharged before implementing the nursing interventions. Therefore, the points for implementation and evaluation phases were removed from the final analysis, and their score range laid between 0 - 20. In the present study, descriptive statistics were used to classify the test scores and calculate the mean and standard deviation. Analytic statistics were applied to examine and compare the tests’ mean differences. Statistical analyses were carried out using SPSS Statistics 20 for Windows (IBM Corporation). The significance level was considered 0.05. A Kolmogorov-Smirnova test was used to indicate the data normality.
4. Results
The age of the participants ranged from 19 to 34 years (M = 21 ± 3.71; 45% female, 55% male). The mean scores before and after the virtual education intervention were 0.17 ± 0.14 and 1.3 ± 0.27 for ND and 0.01 ± 0.6 and 1.29 ± 0.27 for nursing outcomes/goals with overall scores of 0.19 ± 0.17 and 2.65 ± 36, respectively, out of 3 points. The paired-samples t-test results showed a significant difference in the scores for ND (M = 1.13 ± 0.26), t = 19.81, P < 0.001, the scores for goals (M = 1.28 ± 0.26), t = 21.93, P = 0.001, and overall scores (M = 2.46 ± 0.35), t = 30.09, P < 0.001 before and after the virtual intervention.
In the final step of the study, the overall mean score of NCP was 16.59 ± 2.31, which was higher than the mean score, indicating that the virtual education of NP was effective in a clinical setting. The students' scores ranged from 11.7 to 20. The mean scores were 4.63 ± 0.56 for assessment, 4.26 ± 0.72 for ND, 2.19 ± 0.78 for nursing outcomes/goals, and 5.52 ± 1.62 for nursing intervention phases. Moreover, the students' scores ranged from 3 to 5 for assessment, 2.5 to 5 for nursing diagnosis, 0.5 to 3 for nursing outcomes/goals, and 1.5 to 7 for nursing intervention phases.
5. Discussion
The study results confirmed both hypotheses and indicated that virtual education was positively effective in learning NP and applying it in clinical settings. Similar to findings from previous studies (3, 6), the current study showed that virtual education could be a theoretically and clinically credible method in NP education. Virtual education enhances students’ competency and knowledge in learning NP and helps them prepare for clinical practice. Consistent with McCutcheon et al.’s (2) on nursing students, virtual education is as effective as conventional methods in learning and increasing knowledge.
This study contributes to the current literature by providing evidence that virtual education can engage students in the learning process. In agreement with Patterson et al. (6), virtual education allows students to participate actively, encourages students’ interaction, and improves performance. Moreover, using multimedia tools for instruction also improves students’ cognitive skills, enhance their technological proficiency, and enhance their satisfaction with distance learning. Consistent with De Gagne et al. (9), using virtual education for teaching NP is effective in enhancing clinical reasoning by exploring issues and ideas through improving students’ independence in learning.
Providing the students with virtual education prior to their evaluation encouraged them to reach deep learning in terms of clinical evaluation. By applying their previous knowledge learned through virtual education, the students successfully prepared NCP to tackle genuine cases in small group discussions. In agreement with Kohan et al. (10), virtual education helps students engage in self-directed learning effectively, and as Mosalanejad and Sobhanian (8) reported, it improves their skills in critical thinking. Innovative strategies are critical for utilizing the nursing education system to support uninterrupted education and assessment. In this regard, motivation from the instructor is vital to ease frustration among students and create a positive environment for learning to gradually develop students’ acceptance, achieve a new level of performance, and sustain them in task engagement.
Attitudes toward virtual learning are also crucial in creating a suitable environment for instruction (11). Instructors' satisfaction with multimedia instruction as an educational tool is essential in creating a positive attitude toward virtual learning environments, which can motivate them to use virtual education as an effective teaching platform. Toward this end, both instructors and students are provided with adequate technical support to increase their satisfaction in using virtual education platforms. Moreover, consistent with De Gagne et al. (9), the overall success of educational experience depends on facilitating a sense of belonging and creating a safe environment. Proposing a particular scope of teaching tasks when a nursing educator starts a virtual classroom program helps both instructors and students create a safe environment and enhance a sense of belonging.
Limitations of the current study include the lack of control over the students’ access to NP references before they took the pre-tests and the possible influence of references other than those provided by the course content. Moreover, due to the small sample size, a robust generalization of the findings cannot be drawn. Finally, the method used to score the pre- and post-tests limits the study’s findings.
5.1. Conclusion
Virtual education can be an effective method for NP education both theoretically and clinically. It can improve learning outcomes and allow nursing students to keep pace with a changing environment. Virtual education is likely to make nursing students more adaptive to change and help them tackle challenges in a dynamic environment. Continuously improving virtual learning environments can enhance educators’ satisfaction level and encourage them to constantly update themselves in using such environments. This can subsequently influence students’ perceived benefits of virtual education in the long run. Finally, although we used Navid in the present study, education intervention is possible in other types of virtual environments as well.
Acknowledgements
References
-
1.
Giddens J, Fogg L, Carlson-Sabelli L. Learning and engagement with a virtual community by undergraduate nursing students. Nurs Outlook. 2010;58(5):261-7. [PubMed ID: 20934081]. https://doi.org/10.1016/j.outlook.2010.08.001.
-
2.
McCutcheon K, Lohan M, Traynor M, Martin D. A systematic review evaluating the impact of online or blended learning vs. face-to-face learning of clinical skills in undergraduate nurse education. J Adv Nurs. 2015;71(2):255-70. [PubMed ID: 25134985]. https://doi.org/10.1111/jan.12509.
-
3.
Voutilainen A, Saaranen T, Sormunen M. Conventional vs. e-learning in nursing education: A systematic review and meta-analysis. Nurse Educ Today. 2017;50:97-103. [PubMed ID: 28038371]. https://doi.org/10.1016/j.nedt.2016.12.020.
-
4.
Mishra L, Gupta T, Shree A. Online teaching-learning in higher education during lockdown period of COVID-19 pandemic. Int J Educ Res Open. 2020;1:100012. https://doi.org/10.1016/j.ijedro.2020.100012.
-
5.
Sahu P. Closure of Universities Due to Coronavirus Disease 2019 (COVID-19): Impact on Education and Mental Health of Students and Academic Staff. Cureus. 2020;12(4). e7541. [PubMed ID: 32377489]. [PubMed Central ID: PMC7198094]. https://doi.org/10.7759/cureus.7541.
-
6.
Patterson BJ, Krouse AM, Roy L. Student outcomes of distance learning in nursing education: An integrative review. Comput Inform Nurs. 2012;30(9):475-88. [PubMed ID: 22592452]. https://doi.org/10.1097/NXN.0b013e3182573ad4.
-
7.
Quispe-Prieto S, Cavalcanti-Bandos MF, Caipa-Ramos M, Paucar-Caceres A, Rojas-Jiménez HH. A Systemic Framework to Evaluate Student Satisfaction in Latin American Universities under the COVID-19 Pandemic. Systems. 2021;9(1):15. https://doi.org/10.3390/systems9010015.
-
8.
Mousavinasab ES, Rostam Niakan Kalhori S, Zarifsanaiey N, Rakhshan M, Ghazisaeedi M. Nursing process education: A review of methods and characteristics. Nurse Educ Pract. 2020;48:102886. [PubMed ID: 32961511]. https://doi.org/10.1016/j.nepr.2020.102886.
-
9.
De Gagne JC, Oh J, Kang J, Vorderstrasse AA, Johnson CM. Virtual worlds in nursing education: A synthesis of the literature. J Nurs Educ. 2013;52(7):391-6. [PubMed ID: 23755942]. https://doi.org/10.3928/01484834-20130610-03.
-
10.
Kohan N, Soltani Arabshahi K, Mojtahedzadeh R, Abbaszadeh A, Rakhshani T, Emami A. Self- directed learning barriers in a virtual environment: A qualitative study. J Adv Med Educ Prof. 2017;5(3):116-23. [PubMed ID: 28761885]. [PubMed Central ID: PMC5522903].
-
11.
Huang H, Liaw S, Lai C. Exploring learner acceptance of the use of virtual reality in medical education: A case study of desktop and projection-based display systems. Interact Learn Environ. 2013;24(1):3-19. https://doi.org/10.1080/10494820.2013.817436.