Abstract
Background:
Cryptosporidium is one of the most important causes of gastroenteritis in humans.Objectives:
This study aimed to investigate the distribution of Cryptosporidium species in children with acute diarrheal disease in Zahedan, Iran.Methods:
Stool specimens collected from 764 children aged < 10 years with diarrheal disease admitted to Aliasghar Pediatric Hospital and the Reference Laboratory in Zahedan were assessed for the presence of Cryptosporidium oocysts using the conventional microscopic examination and acid-fast staining. To characterize the oocysts at the molecular level, the 18S rRNA was nested-PCR amplified and sequenced. PCR products were also digested using Vsp1 restriction enzyme for genotype differentiation.Results:
Of the 764 stool specimens, 7 (0.91%) were positive for Cryptosporidium oocysts using the microscopic examination. Restriction endonuclease digestion pattern successfully revealed the presence of Cryptosporidium parvum in two microscopic positive samples that were confirmed by DNA sequencing.Conclusions:
Cryptosporidium parvum is responsible for cryptosporidiosis in children under 10 years of age in the study region. Although C. parvum may be an important pathogen associated with diarrhea, it is the cause of only a small proportion of diarrheal episodes.Keywords
1. Background
Cryptosporidium is recognized as an important and common cause of diarrhea in both animals and humans (1). In immunocompetent hosts, it may produce self-limiting acute diarrheal disease. Young animals and children under five years of age are most often infected with this genus. In immunocompromised patients, it may also cause a prolonged severe disease. This coccidium is a major opportunistic pathogen in AIDS patients (2-12). Cryptosporidium oocysts in fecal samples are characterized via microscopic examination after concentrating using different methods, including flotation and formol-ether concentration techniques. To characterize these species, new tools have been introduced in molecular biology (13). Of the 31 Cryptosporidium species that have been recognized as valid, more than 20 species and genotypes are identified in humans, including Cryptosporidium hominis, C. parvum, C. meleagridis, C. felis, C. canis, C. cuniculus, C. ubiquitum, C. viatorum, C. muris, C. suis, C. fayeri, C. andersoni, C. bovis, C. scrofarum, C. tyzzeri, C. erinacei, and Cryptosporidium horse, skunk, and chipmunk I genotypes, with C. hominis and C. parvum being the most commonly reported ones (14, 15).
2. Objectives
Despite previous reports of Cryptosporidium species in Iran (16-20), there is no information on the molecular evaluation of species infecting humans in Zahedan, southwest of Iran. Therefore, this study aimed at identifying these species in children aged < 10 years in the study region.
3. Methods
3.1. Study Population
This study was performed from August 2016 to August 2018 among 764 children with the acute diarrheal disease under 10 years of age, who were admitted to Aliasghar Pediatric Hospital and the Reference Laboratory of Zahedan, Sistan and Baluchestan, Iran. Children attending these hospitals came from different urban and rural areas of the province and they all resided in poor regions. An evaluation was made on each patient at the time of sample collection based on the information provided by the children’s mothers and a review of the patients’ medical histories. The inclusion criteria included an age of ≤ 10 years and no history of antiparasitic drug use during two weeks before the test. The exclusion criteria included children suffering from gastrointestinal disorders including diarrhea, stomach pain, bloating, and nausea or vomiting.
3.2. Fecal Samples
The fecal samples were collected in cardboard boxes within two days of hospital admission or when the child presented as an outpatient. A stool container was given to the mother and she was asked to return a stool sample on the next day. The specimens were then transferred to our laboratory and concentrated using a water-ether concentration procedure.
3.3. Microscopic Examination
For identifying and recovering Cryptosporidium oocysts, the water-ether concentrated stool samples were microscopically examined at 1000X magnification after modified acid-fast staining (21-23).
3.4. DNA Extraction
For DNA extraction, a FavorPrep® Stool DNA Extraction Kit (Favorgen, Taiwan) was used based on the manufacturer’s protocols.
3.5. PCR Amplification
For the amplification of the 18S rRNA gene, a nested PCR protocol was applied, as previously described (24). A C. parvum-positive control was also included to validate the results. The positive sample for C. parvum (previously identified by PCR-RFLP) used in the assays was a gift from Dr. Hadi Mirahmadi, ZAUMS, Zahedan, Iran.
3.6. RFLP Assay
For RFLP analysis, the secondary PCR products were digested with restriction enzyme Vsp1. Horizontal electrophoresis was performed to separate the restriction fragments in the 2% agarose gel.
3.7. Sequence Analysis
A purification kit was used to purify the secondary PCR amplicons (Bioneer, Daejeon, South Korea). An automated DNA analyzer was also used for sequencing in both directions (ABI 3730 XL, Bioneer, South Korea). The sequences were edited manually in BioEdit (http://www.mbio.ncsu.edu/BioEdit/page2.html) and aligned with reference sequences for genotype identification in BLASTN software (http://blast.ncbi.nlm.nih.gov/Blast.cgi). The multiple-sequence alignment was carried out and a phylogenetic tree was plotted using Clustal W and neighbor-joining (NJ) method based on the Kimura two-parameter model in MEGA version 6.0 (25). The bootstrap method was used to evaluate the reliability of the NJ tree with 1000 replicates.
4. Results
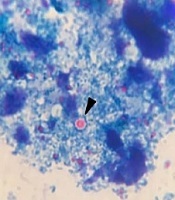
Of 764 stool samples, 0.91% (7/764) were positive for Cryptosporidium oocysts presenting as particles in the microscopic examination (Figure 1A). Overall, 28.6% (2/7) of the positive samples were successfully DNA amplified via nested PCR. The 830-bp products obtained from the secondary PCR were in accordance with the positive control sample (Figure 1B). The expected product was not produced by negative controls based on the nested PCR. No amplification was observed for five microscopically positive fecal samples.
A, Cryptosporidium spp. oocyst-like particles detected in stool specimens of symptomatic patients in the current study (scale bar, 10 μm); B, nested-PCR products on the ethidium bromide-stained 2% agarose gel. Lanes 1 and 4: C. parvum-positive samples (830 bp fragment); lanes 2 and 3: negative samples; lane N: negative control; lane P: positive control; lane L: 100-bp DNA ladder (Cinnagen/Iran); C, gel electrophoresis of DNA fragments obtained after digestion with Vsp1 restriction enzyme. Lanes 1 and 2 (positive samples) and P (positive control) show the banding patterns after digestion with Vsp1 (GenBank Accession no. MK530165, MK530166, and MK530167); lane L is a 100-bp DNA ladder.

The secondary PCR products, which were exposed to Vsp1 restriction enzyme digestion, indicated the presence of C. parvum in the positive control and fecal samples, as gel electrophoresis indicated two bands with sizes of 100 bp and 628 bp (Figure 1C). The PCR-positive fecal and positive-control samples were successfully sequenced. In total, 23 nucleotide sequences were included in the analysis (Figure 2). According to the search of 18S rRNA sequences (560 bp - 815 bp) against the published sequences of other Cryptosporidium species, the greatest homology was attributed to C. parvum (99% - 100%). The nucleotide sequences in our study were deposited in GenBank (accession No., MK530165 and MK530166). Moreover, the nucleotide sequence of the positive control sample was deposited in GenBank (No., MK530167).
Phylogenetic tree based on 18S sequences, constructed according to the NJ method, showing the position of Cryptosporidium species. Cystoisospora suis and Eimeria spp. were used as outgroups. The percentage of replicate tree in which the associated taxa were clustered together in the bootstrap test (1,000 replicates) is shown next to the branches.

5. Discussion
The present study showed that C. parvum is an important cause of diarrhea in children younger than 10 years in Zahedan, Iran. This finding was not unexpected, as intestinal parasites are common in this area and the studied population represented the lowest income class in the region, with poor environmental sanitation facilitating frequent exposure to enteropathogens. The prevalence of cryptosporidiosis has been examined in diarrhea children in different areas of Iran. In studies by Keshavarz et al. (17) and Saneian et al. (18), low prevalence rates were reported in the central regions of Iran (2.5% and 4.6%, respectively). On the other hand, Mirzaei (19) reported a high prevalence rate in the southern regions of Iran (35%). In a study by Dabirzadeh et al. (20) from Zabol, microscopic examinations indicated the rate of positive samples as 9.5% (19/200). The findings represent geographical differences in the prevalence of Cryptosporidium in Iran.
Microscopic examination is commonly used to detect Cryptosporidium oocysts in fecal samples after concentrating using different methods, including flotation and formol-ether concentration techniques. The efficacy of molecular methods has been confirmed for the identification and classification of Cryptosporidium oocysts. In the present study, nested-PCR and RFLP assays were conducted to identify Cryptosporidium species in stool samples. The rate of positivity was lower in PCR than in microscopic examination. Previous studies also reported similar findings, which might be attributed to DNA inadequacy due to the low number of oocysts in stool samples (26-28).
Cryptosporidium parvum and C. hominis are usually responsible for the disease in humans. Although other animals, especially cattle, and humans are the reservoir hosts for C. parvum, humans are the only reservoirs for C. hominis. In addition, the distribution of these infective parasitic species varies in different countries. A previous study showed that C. parvum accounted for most cases of the disease among humans in the United Kingdom (61.5%) (29). In addition, different seasonal patterns were reported for these species. The peak of C. parvum infection occurs in the late spring while the peak of C. hominis infection is in the fall (30). The present study was conducted from August 2016 to August 2018. Evidence suggests that C. hominis accounts for most human infections in the United States, Kenya, Guatemala, Australia, and Peru (31-33). In Iran and its neighboring countries, C. parvum is more frequently reported than C. hominis (33-36). Cryptosporidium was identified in 4 out of 707 school children from Turkey (0.6%); all the isolates belonged to the C. parvum bovine genotype (34). The current results are consistent with the reports from Saudi Arabia, Iran, Kuwait, and Turkey (8, 22-36).
Cattle are a major source of zoonotic cryptosporidiosis with C. parvum. Some of the transmission routes include direct contact with infected calves and water contamination with the cattle manure (37). According to a survey from Northwestern regions of Iran, C. parvum and C. andersoni infected 10.5% of the cattle (38). However, the transmission route cannot be achieved by the determination of species. Some of the C. parvum subtypes are found only in humans, indicating that some of these subtypes have anthroponotic transmission and some others are zoonotic (39).
5.1. Conclusions
We evaluated the distribution of cryptosporidial infection in children (< 10-years-old) in Zahedan, Iran. The presence of this infection in children can be threatening to other susceptible people in this region. Nevertheless, it is important to conduct further epidemiological studies to evaluate the risk of cryptosporidial infection in other susceptible people, including immunocompromised patients.
Acknowledgements
References
-
1.
Saaed FMA, Ongerth JE. Giardia and Cryptosporidium in children with diarrhea, Kufra, Libya, a North African migration route city. Int J Hyg Environ Health. 2019;222(5):840-6. [PubMed ID: 31085111]. https://doi.org/10.1016/j.ijheh.2019.04.006.
-
2.
Wang RJ, Li JQ, Chen YC, Zhang LX, Xiao LH. Widespread occurrence of Cryptosporidium infections in patients with HIV/AIDS: Epidemiology, clinical feature, diagnosis, and therapy. Acta Trop. 2018;187:257-63. [PubMed ID: 30118699]. https://doi.org/10.1016/j.actatropica.2018.08.018.
-
3.
Ghafari R, Rafiei A, Tavalla M, Moradi Choghakabodi P, Nashibi R, Rafiei R. Prevalence of Cryptosporidium species isolated from HIV/AIDS patients in southwest of Iran. Comp Immunol Microbiol Infect Dis. 2018;56:39-44. [PubMed ID: 29406282]. https://doi.org/10.1016/j.cimid.2017.12.002.
-
4.
Sannella AR, Suputtamongkol Y, Wongsawat E, Caccio SM. A retrospective molecular study of Cryptosporidium species and genotypes in HIV-infected patients from Thailand. Parasit Vectors. 2019;12(1):91. [PubMed ID: 30867022]. [PubMed Central ID: PMC6417249]. https://doi.org/10.1186/s13071-019-3348-4.
-
5.
Mor SM, Ascolillo LR, Nakato R, Ndeezi G, Tumwine JK, Okwera A, et al. Expectoration of Cryptosporidium parasites in sputum of human immunodeficiency virus-positive and -negative adults. Am J Trop Med Hyg. 2018;98(4):1086-90. [PubMed ID: 29405104]. [PubMed Central ID: PMC5928827]. https://doi.org/10.4269/ajtmh.17-0741.
-
6.
Golan Shaposhnik E, Abozaid S, Grossman T, Marva E, On A, Azrad M, et al. The prevalence of Cryptosporidium among children hospitalized because of gastrointestinal symptoms and the efficiency of diagnostic methods for Cryptosporidium. Am J Trop Med Hyg. 2019;101(1):160-3. [PubMed ID: 31115293]. [PubMed Central ID: PMC6609172]. https://doi.org/10.4269/ajtmh.19-0057.
-
7.
El-Kady AM, Fahmi Y, Tolba M, Hashim AA, Hassan AA. Cryptosporidium infection in chronic kidney disease patients undergoing hemodialysis in Egypt. J Parasit Dis. 2018;42(4):630-5. [PubMed ID: 30538364]. [PubMed Central ID: PMC6261133]. https://doi.org/10.1007/s12639-018-1046-3.
-
8.
Mahmoudi MR, Ongerth JE, Karanis P. Cryptosporidium and cryptosporidiosis: The Asian perspective. Int J Hyg Environ Health. 2017;220(7):1098-109. [PubMed ID: 28760503]. https://doi.org/10.1016/j.ijheh.2017.07.005.
-
9.
Chavez MA, White AJ. Novel treatment strategies and drugs in development for cryptosporidiosis. Expert Rev Anti Infect Ther. 2018;16(8):655-61. [PubMed ID: 30003818]. https://doi.org/10.1080/14787210.2018.1500457.
-
10.
Vanathy K, Parija SC, Mandal J, Hamide A, Krishnamurthy S. Cryptosporidiosis: A mini review. Trop Parasitol. 2017;7(2):72-80. [PubMed ID: 29114483]. [PubMed Central ID: PMC5652058]. https://doi.org/10.4103/tp.TP_25_17.
-
11.
Vanathy K, Parija SC, Mandal J, Hamide A, Krishnamurthy S. Detection of Cryptosporidium in stool samples of immunocompromised patients. Trop Parasitol. 2017;7(1):41-6. [PubMed ID: 28459014]. [PubMed Central ID: PMC5369273]. https://doi.org/10.4103/tp.TP_66_16.
-
12.
Barcelos NB, Silva LFE, Dias RFG, Menezes Filho HR, Rodrigues RM. Opportunistic and non-opportunistic intestinal parasites in HIV/ AIDS patients in relation to their clinical and epidemiological status in a specialized medical service in Goias, Brazil. Rev Inst Med Trop Sao Paulo. 2018;60. e13. [PubMed ID: 29538510]. [PubMed Central ID: PMC5962243]. https://doi.org/10.1590/S1678-9946201860013.
-
13.
Fallahi S, Moosavi SF, Karimi A, Chegeni AS, Saki M, Namdari P, et al. An advanced uracil DNA glycosylase-supplemented loop-mediated isothermal amplification (UDG-LAMP) technique used in the sensitive and specific detection of Cryptosporidium parvum, Cryptosporidium hominis, and Cryptosporidium meleagridis in AIDS patients. Diagn Microbiol Infect Dis. 2018;91(1):6-12. [PubMed ID: 29366630]. https://doi.org/10.1016/j.diagmicrobio.2017.12.017.
-
14.
Ryan U, Zahedi A, Paparini A. Cryptosporidium in humans and animals-a one health approach to prophylaxis. Parasite Immunol. 2016;38(9):535-47. [PubMed ID: 27454991]. https://doi.org/10.1111/pim.12350.
-
15.
Feng Y, Xiao L. Molecular epidemiology of Cryptosporidiosis in China. Front Microbiol. 2017;8:1701. [PubMed ID: 28932217]. [PubMed Central ID: PMC5592218]. https://doi.org/10.3389/fmicb.2017.01701.
-
16.
Hamedi Y, Safa O, Haidari M. Cryptosporidium infection in diarrheic children in southeastern Iran. Pediatr Infect Dis J. 2005;24(1):86-8. [PubMed ID: 15665718]. https://doi.org/10.1097/01.inf.0000148932.68982.ec.
-
17.
Keshavarz A, Athari A, Haghighi A, Kazami B, Abadi A, Nazemalhoseini Mojarad E, et al. Genetic characterization of Cryptosporidium spp. among children with diarrhea in Tehran and Qazvin provinces, Iran. Iran J Parasitol. 2008;3(3):30-6.
-
18.
Saneian H, Yaghini O, Yaghini A, Modarresi MR, Soroshnia M. Infection rate of Cryptosporidium parvum among diarrheic children in Isfahan. Iran J Pediatr. 2010;20(3):343-7. [PubMed ID: 23056727]. [PubMed Central ID: PMC3446045].
-
19.
Mirzaei M. Prevalence of Cryptosporidium sp. infection in diarrheic and non-diarrheic humans in Iran. Korean J Parasitol. 2007;45(2):133-7. [PubMed ID: 17570977]. [PubMed Central ID: PMC2526311]. https://doi.org/10.3347/kjp.2007.45.2.133.
-
20.
Dabirzadeh M, Rostami D, Bagheri S. Prevalence of Cryptosporidium species in children referred to central and hospital laboratories of Zabol city, south east of Iran. Int JPediatr. 2017;5(12):6359-64. https://doi.org/10.22038/ijp.2017.22358.1871.
-
21.
Hatam-Nahavandi K, Mahvi AH, Mohebali M, Keshavarz H, Mobedi I, Rezaeian M. Detection of parasitic particles in domestic and urban wastewaters and assessment of removal efficiency of treatment plants in Tehran, Iran. J Environ Health Sci Eng. 2015;13:4. [PubMed ID: 25653867]. [PubMed Central ID: PMC4316801]. https://doi.org/10.1186/s40201-015-0155-5.
-
22.
Hatam-Nahavandi K, Mohebali M, Mahvi AH, Keshavarz H, Mirjalali H, Rezaei S, et al. Subtype analysis of Giardia duodenalis isolates from municipal and domestic raw wastewaters in Iran. Environ Sci Pollut Res Int. 2017;24(14):12740-7. [PubMed ID: 26965275]. https://doi.org/10.1007/s11356-016-6316-y.
-
23.
Fallah E, Nahavandi KH, Jamali R, Mahdavi B, Asgharzadeh M. Genetic characterization of Giardia intestinalis strains from patients having sporadic giardiasis by using PCR assay. J Med Sci. 2008;8(3):310-5. https://doi.org/10.3923/jms.2008.310.315.
-
24.
Jiang J, Alderisio KA, Xiao L. Distribution of cryptosporidium genotypes in storm event water samples from three watersheds in New York. Appl Environ Microbiol. 2005;71(8):4446-54. [PubMed ID: 16085835]. [PubMed Central ID: PMC1183313]. https://doi.org/10.1128/AEM.71.8.4446-4454.2005.
-
25.
Kumar S, Stecher G, Tamura K. MEGA7: Molecular evolutionary genetics analysis version 7.0 for bigger datasets. Mol Biol Evol. 2016;33(7):1870-4. [PubMed ID: 27004904]. https://doi.org/10.1093/molbev/msw054.
-
26.
Hatam-Nahavandi K, Mohebali M, Mahvi AH, Keshavarz H, Najafian HR, Mirjalali H, et al. Microscopic and molecular detection of Cryptosporidium andersoni and Cryptosporidium xiaoi in wastewater samples of Tehran province, Iran. Iran J Parasitol. 2016;11(4):499-506. [PubMed ID: 28127361]. [PubMed Central ID: PMC5251178].
-
27.
Hatam Nahavandi K, Mahvi AH, Mohebali M, Keshavarz H, Rezaei S, Mirjalali H, et al. Molecular typing of Eimeria ahsata and E. crandallis isolated from slaughterhouse wastewater. Jundishapur J Microbiol. 2016;9(4). e34140. [PubMed ID: 27303617]. [PubMed Central ID: PMC4902853]. https://doi.org/10.5812/jjm.34140.
-
28.
Hatam-Nahavandi K, Mohebali M, Mahvi AH, Keshavarz H, Khanaliha K, Tarighi F, et al. Evaluation of Cryptosporidium oocyst and Giardia cyst removal efficiency from urban and slaughterhouse wastewater treatment plants and assessment of cyst viability in wastewater effluent samples from Tehran, Iran. J Water Reuse Desalination. 2015;5(3):372-90. https://doi.org/10.2166/wrd.2015.108.
-
29.
McLauchlin J, Amar C, Pedraza-Diaz S, Nichols GL. Molecular epidemiological analysis of Cryptosporidium spp. in the United Kingdom: Results of genotyping Cryptosporidium spp. in 1,705 fecal samples from humans and 105 fecal samples from livestock animals. J Clin Microbiol. 2000;38(11):3984-90. [PubMed ID: 11060056]. [PubMed Central ID: PMC87529].
-
30.
Jagai JS, Castronovo DA, Monchak J, Naumova EN. Seasonality of cryptosporidiosis: A meta-analysis approach. Environ Res. 2009;109(4):465-78. [PubMed ID: 19328462]. [PubMed Central ID: PMC2732192]. https://doi.org/10.1016/j.envres.2009.02.008.
-
31.
Xiao L, Escalante L, Yang C, Sulaiman I, Escalante AA, Montali RJ, et al. Phylogenetic analysis of Cryptosporidium parasites based on the small-subunit rRNA gene locus. Appl Environ Microbiol. 1999;65(4):1578-83. [PubMed ID: 10103253]. [PubMed Central ID: PMC91223].
-
32.
Ramirez NE, Ward LA, Sreevatsan S. A review of the biology and epidemiology of cryptosporidiosis in humans and animals. Microbes Infect. 2004;6(8):773-85. [PubMed ID: 15207825]. https://doi.org/10.1016/j.micinf.2004.02.021.
-
33.
Sulaiman IM, Hira PR, Zhou L, Al-Ali FM, Al-Shelahi FA, Shweiki HM, et al. Unique endemicity of cryptosporidiosis in children in Kuwait. J Clin Microbiol. 2005;43(6):2805-9. [PubMed ID: 15956401]. [PubMed Central ID: PMC1151898]. https://doi.org/10.1128/JCM.43.6.2805-2809.2005.
-
34.
Tamer GS, Turk M, Dagci H, Pektas B, Guy EC, Guruz AY, et al. The prevalence of cryptosporidiosis in Turkish children, and genotyping of isolates by nested polymerase chain reaction-restriction fragment length polymorphism. Saudi Med J. 2007;28(8):1243-6. [PubMed ID: 17676211].
-
35.
Areeshi MY, Beeching NJ, Hart CA. Cryptosporidiosis in Saudi Arabia and neighboring countries. Ann Saudi Med. 2007;27(5):325-32. [PubMed ID: 17921688]. [PubMed Central ID: PMC6077050]. https://doi.org/10.5144/0256-4947.2007.325.
-
36.
Taghipour N, Nazemalhosseini-Mojarad E, Haghighi A, Rostami-Nejad M, Romani S, Keshavarz A, et al. Molecular epidemiology of cryptosporidiosis in Iranian children, Tehran, Iran. Iran J Parasitol. 2011;6(4):41-5. [PubMed ID: 22347312]. [PubMed Central ID: PMC3279909].
-
37.
Xiao L, Feng Y. Zoonotic cryptosporidiosis. FEMS Immunol Med Microbiol. 2008;52(3):309-23. [PubMed ID: 18205803]. https://doi.org/10.1111/j.1574-695X.2008.00377.x.
-
38.
Fallah E, Mahdavi Poor B, Jamali R, Hatam Nahavandi K, Asgharzadeh M. Molecular characterization of Cryptosporidium isolates from cattle in a slaughterhouse in Tabriz, Northwestern Iran. J Biol Sci. 2008;8(3):639-43. https://doi.org/10.3923/jbs.2008.639.643.
-
39.
King P, Tyler KM, Hunter PR. Anthroponotic transmission of Cryptosporidium parvum predominates in countries with poorer sanitation: A systematic review and meta-analysis. Parasit Vectors. 2019;12(1):16. [PubMed ID: 30621759]. [PubMed Central ID: PMC6323761]. https://doi.org/10.1186/s13071-018-3263-0.