Abstract
Background:
The cesarean section plays an important role in reducing mortality rates and postpartum complications in the mother and fetus in certain deliveries.Objectives:
The aim of this study was to determine the effect of magnesium sulfate supplementation on intrathecal marcain on pain control after cesarean section.Methods:
This randomized clinical trial study was performed on 42 women candidates for cesarean section in Vali-e-Asr Hospital in Birjand in 2018. In each group, vital signs and pain score were assessed every 15 minutes using the Visual Intensity Pain Scale (VAS) 1,2,3,4,8,12 hours after surgery. Data were collected and analyzed using the Friedman test, t-test for independent groups, Mann-Whitney, and chi-square by SPSS software.Results:
The mean age of women candidates for cesarean section was 29.11 ± 5.42 years. The mean VAS score in both groups at different times was statistically significant. At 1 and two hours after surgery, the mean VAS score in magnesium sulfate and marcaine groups was significantly higher than marcaine group and in three hours after the surgery, it was significantly less than the Marcain group but there was no significant difference in other times. Changes in pain intensity in the magnesium sulfate and marcaine groups were significantly greater than the marcaine group.Conclusions:
Addition of magnesium sulfate to intrathecal marcaine has a significant effect on pain management after cesarean section.Keywords
1. Background
The cesarean section plays an important role in reducing mortality rates and postpartum complications in the mother and fetus in certain deliveries. The complications include pain, wound infection, bleeding, aspiration, pulmonary atelectasis, lung airway infections, and pulmonary embolism (1).
Postoperative pain is controlled by many methods, including systemic (opioids and non-opioids) and local (neuraxial and peripheral) analgesia techniques (2).
Undoubtedly, it is of paramount importance to find methods with minimal unwanted side effects, along with proper pain control (3). Different systemic and regional methods are nowadays used for postoperative analgesia, among which regional methods are superior due to the reduction of complications (2).
In regional methods, various adjuvant compounds are used to help patients achieve analgesia. Inclusion of compounds, such as ketamine, fentanyl, prostigmin, midazolam, clonidine, etc., into local anesthetics in spinal anesthesia is associated with disadvantages, in addition to their benefits, making their use limited and sometimes impossible (4).
Magnesium (Mg), a physiological blocker of calcium channels and a non-competitive antagonist of N-methyl disapartate (NMDA) receptors, can exert pain control effects by inhibiting central sensitization to pain (4). This drug exerts pain control effects in the medullary axis. Numerous clinical studies have demonstrated that magnesium sulfate (MgSO4) infusion during general anesthesia reduces the need for intraoperative anesthesia and postoperative analgesics (5), while some other studies suggest that magnesium administration close to the operation slightly affects postoperative pain (6, 7). This drug exerts pain control effects on the medullary axis. Intravenous administration of MgSO4 during general anesthesia reduces the intra- and postoperative need for narcotics (8, 9). Another analgesic drug is bupivacaine (marcaine), which is a long-acting amide-type local anesthetic (10), is available at a concentration of 0.5%, causes good analgesia, and is also accessible and inexpensive (11, 12).
Cesarean section is important in several aspects because not only the mother but also the newborn needs maternal care in the first days after birth. Pain is an impediment to the mother in supporting the newborn, in particular breastfeeding. Therefore, postoperative pain reduction is considered an important factor for both physicians and patients (5). Because of the importance of this topic, our study aimed to compare the effect of adding MgSO4 to intrathecal marcaine on pain control after cesarean section.
2. Objectives
This research actually compared analgesia in patients under spinal anesthesia with marcaine and a combination of MgSO4 and marcaine.
3. Methods
This randomized clinical trial was approved by the ethics committee of Birjand University of Medical Sciences (with the code ir.bums.REC.1396.320) and IRCT code (IRCT20190123042473N1) conducted at Vali-e-Asr Hospital (Birjand city) in 2017. The participants consisted of 42 pregnant women who were candidates for non-emergency cesarean section. Inclusion criteria were ages of 15-45 years, being in ASA I II (the class of American Society of Anesthesiologists), insensitivity to amide anesthetics, and no contraindications to spinal anesthesia, lack of other underlying conditions such as heart disease, coagulation, or infectious disease, no history of psychotropic drugs, and non-smokers. Patients undergoing surgery for more than 30 min that required another surgery (e.g. myomectomy or cystectomy) during cesarean section, or underwent atony or another unforeseen event after the surgery were excluded from the study.
Cesarean section patients referred to Vali-e-Asr Hospital, who met the inclusion criteria, were recruited by the convenience sampling method. The subjects were randomly assigned to one of the MgSO4 and marcaine-marcaine (M-M) groups. Before the surgery, each patient was drawn by choosing one of the red or green cards before entering the operating room. Patients who selected the red card were assigned to group M (marcaine + MgSO4) and received 10 mg of 0.5% M and 80 mg of MgSO4. Subjects who selected a green card were allocated to group C (marcaine) and received only 10 mg of 0.5% intrathecal marcaine.
All patients received 10 cc/kg of an intravenous crystalloid solution and underwent spinal anesthesia at the L3-L4 or L4-L5 vertebral levels with needle No. 25 by an anesthetist. Immediately after spinal anesthesia injection, the patient was placed in a supine position and supplied with nasal oxygen at 4-5 L/min. The patients were monitored by a Saadat monitoring device equipped with non-invasive blood pressure measurement that recorded ECG and measured pulse oximetry. All post-injection evaluations were done by an anesthesia resident (technician) who was completely unaware of injectable drugs. Vital signs, such as blood pressure and heart rate, were recorded every 5-30 min (after the injection) and then every 15 min until the end of the operation. Pain scores were evaluated at 1, 2, 3, 4, 8, and 12 h after the surgery. In the case of hypotension (SBP < 90) or more than a 20% drop of baseline blood pressure, patients were injected with 250 cc of Berlus normal saline and, in the case of no response, 10 mg of ephedrine was injected to patients. Atropine (0.5 mg) was administered for decreased heart rate (< 50/mm) and if it did not respond, the injection was repeated up to three times with the same dose; adrenaline was administered with the continued conditions. The duration of analgesia was recorded from the time of intrathecal drug injection until the first request for an analgesic by the patient. Intravenous pethidine (0.5 mg/kg) was prescribed upon the request for an analgesic (VAS > 4). Postoperative pain intensity was re-determined using a VAS graduated system by asking the patient by a trained person every hour post-operation for up to 4 h and then every 4 h for up to 12 h, that is, pain intensity was recorded at 8, 4, 3, 2, 1, and 12 h after the surgery. These special hours were chosen to consider the time limit of the maximum action duration of the drugs. During this period, the complaint of pain was recorded in the case of VAS > 4 or pain expression by the patient.
Patients’ information, including gender, age, urinary retention, 1 min neonatal Apgar score, 5 min neonatal Apgar score, and clinical signs, were recorded in a researcher-made checklist and analyzed by SPSS 22 software using descriptive and analytical statistical analyses. Data analysis by descriptive statistics, including frequency tables, central tendency, and dispersion, aimed to describe the most important characteristics of the subjects. Quantitative and qualitative data were reported as mean ± standard deviation (SD) and a number (%), respectively. Between-group comparisons were made using the Friedman test in multiple measurements. Depending on the normality or non-normality of data, other between-group comparisons were performed using Chi-square, two-sample independent t-test, and Mann-Whitney tests. The normality of variables was evaluated by the Shapiro-Wilk test. A significance level of 0.05 was considered in all tests.
4. Results
In this study, the included participants were 42 women candidates for cesarean section, all of whom were followed up until the end of the study. The age of patients ranged between 17 and 39 years with a mean (± SD) age of 29.11 ± 5.42 years.
The intrathecal M and MgSO4 + intrathecal M groups were not significantly different in terms of hemodynamic characteristics at the beginning of the study (Table 1). The 1 min neonatal Apgar score was only significantly higher in the intrathecal M group than in MgSO4 + intrathecal M patients (Table 1).
Comparison of Hemodynamic Characteristics at the Beginning of the Study Between the Two Groups of Intrathecal Marcaine and Magnesium Sulfate with Intrathecal Marcaine
| Intrathecal Marcaine, SD ± Average | Magnesium Sulfate with Intrathecal Marcaine, Average ± SD | P Value | |
|---|---|---|---|
| Heart rate | 90.10 ± 17.17 | 89.76 ± 17.55 | 0.95 |
| Systolic blood pressure | 118.76 ± 10.44 | 117.43 ± 9.61 | 0.66 |
| Diastolic blood pressure | 74.05 ± 14.58 | 69.24 ± 7.09 | 0.18 |
| Pregnant age | 38.5 ± 6.88 | 38.92 ± 3.75 | 0.84 |
| Apgar newborn 1 (minute) | 9.67 ± 0.48 | 9.26 ± 0.45 | 0.01 |
| Apgar newborn 5 (minute) | 9.86 ± 0.35 | 10 ± 0.0 | 0.09 |
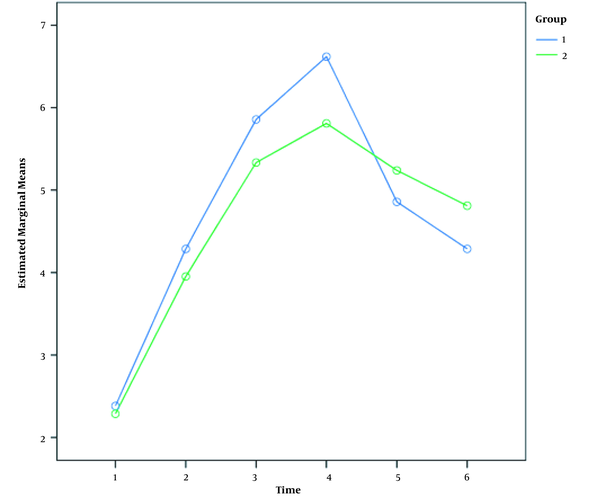
The mean VAS score was statistically significant in both groups at different times (Table 2). At 1 and 2 h post-surgery, the mean VAS score was significantly higher in the MgSO4 + intrathecal M group than in the M group, but it was significantly lower than the M group in 3 h after the surgery. Changes in pain intensity were 3.52 ± 2.18 and 4.23 ± 2.11 in the M and MgSO4 + intrathecal M groups, respectively, which was significantly higher in the latter group (P < 0.05). These changes were first increasing and then decreasing in both groups. The mean of the VAS variable increased up to 4 h post-surgery in both groups and then decreased with a steeper slope in the intrathecal M group than in the MgSO4 + intrathecal M group (Figure 1). This suggests that time can act as an effective factor in postoperative pain reduction in both treatment groups. Moreover, adding MgSO4 significantly affected the pain reduction after cesarean section. Therefore, the observed difference between the two curves (Figure 1) is statistically significant.
Comparison of Mean Vas in Two Groups and Different Times
| Time VAS Score | After One Hour, Mean ± SD | After Two Hour, Mean ± SD | After Three-Hour, Mean ± SD | After Four Hour, Mean ± SD | After 8 Hour, Mean ± SD | After 12 Hour, Mean ± SD | P Value |
|---|---|---|---|---|---|---|---|
| Intrathecal marcaine | 4.29 ± 1.95 | 4.86 ± 1.65 | 6.62 ± 2.03 | 5.86 ± 2.57 | 4.29 ± 2.26 | 2.38 ± 2.01 | < 0.001 |
| Magnesium sulfate with intrathecal marcaine | 4.81± 2.46 | 5.24 ±2.04 | 5.81 ± 1.75 | 5.33 ± 2.15 | 3.95 ± 1.32 | 2.29 ± 1.61 | < 0.001 |
| P value | 0.02 | 0.03 | 0.02 | 0.47 | 0.56 | 0.86 |
Estimated Marginal Means of MEASURE_1
The dose of pethidine used in the intrathecal M group (33.33 ± 22.82) was significantly higher than that in the MgSO4 + intrathecal M group (14.22 ± 18.66) (P = 0.007).
The rates of shivering in recovery were 5 (23.8%) and 3 (14.3%) in the M and MgSO4 + intrathecal M groups, respectively, which was not statistically significant between the two groups (P = 0.69). Urinary retention rates were 12 (57.1%) and 8 (38.1%) in the M and MgSO4 + intrathecal M groups, respectively (P = 0.35).
5. Discussion
One of the most important mental challenges for patients requiring surgical treatments is the intensity and duration of acute postoperative pain, which leads to surgery prevention or delay in most of them. Since surgeons always face this issue, among others, postoperative pain relief has been one of major concerns of medical teams. Therefore, many studies have so far investigated postoperative pain control methods, and different methods have been introduced for this purpose. Postoperative pain reduction accelerates recovery of function, reduces the length of hospital stay, reduces postoperative morbidity, and reduces the possible development of chronic postoperative pain (13).
The cesarean section is important in several aspects because not only the mother but also the newborn needs maternal care in the first days after birth. Pain is an impediment to the mother in supporting newborn, in particular breastfeeding. Therefore, postoperative pain reduction is considered an essential factor for both physicians and patients (5). Because of the importance of this topic, our study aimed to compare the effect of adding MgSO4 to intrathecal marcaine on pain control after the cesarean section.
Our study showed that the average pain in the MgSO4 + intrathecal M group was significantly lower than the intrathecal M group, hence, the addition of MgSO4 significantly influenced pain reduction after cesarean section. The efficacy and safety of different postoperative pain control methods have so far been examined in various studies reporting different results (14-16). Bupivacaine is one of the most widely used drugs in this context with good results. Bærentzen et al. examined the effect of bupivacaine in blocking ilioinguinal and iliohypogastric nerves on pain after inguinal hernia surgery. They found that pain intensity was significantly lower in the bupivacaine group than in the placebo group based on a numerical rating scale (NRS), but the two groups were not different in the need for intravenous morphine and duration of recovery stay. Moreover, the number of patients with acute (NRS > 5) and moderate (NRS > 3) pain was lower in the bupivacaine group (15).
Magnesium is one of the NMDA receptor antagonists and the related ion channels. It can prevent central sensitization and reduce acute sensitivity. Ample evidence has so far been obtained for the analgesic effects of intrathecal Mg in animals. Some human studies have also demonstrated that systemic Mg can have analgesic effects due to its effect on NMDA receptors in the spinal cord. However, there is considerable ambiguity about the transfer of Mg from the blood to the CSF given the blood-brain barrier in normal people, and generally about the mechanism of action of Mg in analgesia (17). MgSO4 is a drug that has been used to control postoperative pain and produced acceptable results in many previous studies (8, 18-20). In a recent meta-analysis, Albertche et al. have reviewed the results of 25 studies that investigated the impact of MgSO4 on postoperative pain compared with placebo. They found that intravenous injection of this drug could be associated with a significant reduction in the need for intravenous morphine (24.4%) during the first 24 h after surgery. They also discovered that MgSO4 injection was associated with a slight decrease in pain score based on the NRS on the first postoperative day at rest or movement. They detected no side effects from MgSO4 injection (18). In another meta-analysis, De Oliveira et al. disclosed that intravenous injection of MgSO4 could reduce opioid use and postoperative pain intensity with no post-injection adverse side effects (21). In Shanghai (China), Chen et al. (2012) evaluated the effect of intra-articular injection of MgSO4 and ropivacaine (RPC) during knee replacement on postoperative pain. In this study, 60 patients were divided into control (normal saline) and case (MgSO4 and RPC) groups. All patients were provided with PCA pumps in the first 48 h after surgery. Collecting data revealed that a significantly lower dose of morphine was used in the case group than in the control group, and patients in the case group experienced much less pain (19). Dabbagh et al. claimed that intravenous and intra-articular injection of MgSO4 could reduce the need for morphine after orthopedic surgery (20). In a study by Turan et al. (22) on 30 patients, adding 10 mL of 15% MgSO4 solution to 0.5% lidocaine solution in regional anesthesia led to shorter sensory and motor block time, longer sensory and motor block recovery time, and less tourniquet pain in patients. In another study on 30 patients, Narang et al. reported that adding 6 ml of 25% MgSO4 solution to 2% lidocaine was effective in sensory and motor block function in regional anesthesia (23). Naderi Nabi et al. presented evidence that painless duration was prolonged by adding 100 mg of MgSO4 to spinal anesthesia without the side effects after orthopedic surgery. The safety of a higher intraspinal dose of MgSO4 was also demonstrated in their study (24).
The present study revealed that the pain intensity gradually increased in both groups with increasing time after the surgery, probably due to the reduced effects of analgesics used during the surgery. On the other hand, the decreased pain intensity in both groups after 4 h can be attributed to a decrease in the release of inflammatory mediators over time. However, in all cases where patients’ pain was measured using VAS, lower pain intensity was recorded in the MgSO4 + intrathecal M group than that of the intrathecal M group.
Acknowledgements
References
-
1.
Gibbs RS, Karlan BY, Haney AF, Nygaard IE. Danforth's obstetrics and gynecology. 2. PA, USA: Lippincott Williams & Wilkins Philadelphia; 2008.
-
2.
Miller RD. Postoperartive Care, Acute Postoperative Pain. Miller's Anesthesia. 7th ed ed. New York: Willams and Wilkins; 2010. p. 2758-71.
-
3.
Koduli B, Oberoi Y, Jones SB; et al. Management of Postoperative Pain. 2010. Available from: https://www.uptodate.com/contents/managementof-postoperative-pain.
-
4.
Bamigboye AA, Hofmeyr GJ. Caesarean section wound infiltration with local anaesthesia for postoperative pain relief - any benefit? S Afr Med J. 2010;100(5):313-9. eng. [PubMed ID: 20460027]. https://doi.org/10.7196/samj.3716.
-
5.
Wilder-Smith O, Hoffmann A, Borgeat A, Rifat K. Fentanyl or Magnesium Analgesic Supplementation of Anesthesia. Anesthesiology. 1992;77(Supplement). https://doi.org/10.1097/00000542-199209001-00208.
-
6.
Ryu JH, Sohn IS, Do SH. Controlled hypotension for middle ear surgery: a comparison between remifentanil and magnesium sulphate. Br J Anaesth. 2009;103(4):490-5. eng. [PubMed ID: 19687032]. https://doi.org/10.1093/bja/aep229.
-
7.
Miller RD. Miller’s Anesthesia text book. Newyork: churchillivingstone; 2010.
-
8.
Tramer MR, Schneider J, Marti RA, Rifat K. Role of magnesium sulfate in postoperative analgesia. Anesthesiology. 1996;84(2):340-7. eng. [PubMed ID: 8602664]. https://doi.org/10.1097/00000542-199602000-00011.
-
9.
Yousef AA, Amr YM. The effect of adding magnesium sulphate to epidural bupivacaine and fentanyl in elective caesarean section using combined spinal-epidural anaesthesia: a prospective double blind randomised study. Int J Obstet Anesth. 2010;19(4):401-4. eng. [PubMed ID: 20833531]. https://doi.org/10.1016/j.ijoa.2010.07.019.
-
10.
Bukhari MA, Al-Saied AS. Evaluation of the effect of Bupivacaine (Marcaine) in reducing early post tonsillectomy pain. Saudi Med J. 2012;33(11):1201-4. eng. [PubMed ID: 23147877].
-
11.
Miller RD. Miller's anesthesia. In: Chales B, Berde Gary R, editors. Local Anesthetics. 7th ed ed. Philadelphia: Churchill Livingstone; 2010. p. 925-30.
-
12.
FDA. Bupivacaine Spinal Official FDA information, side effects and uses. [updated Feb 1, 2021]. Available from: www.drugs.com/pro/bupivacaine-spinal.html.
-
13.
Barreveld A, Witte J, Chahal H, Durieux ME, Strichartz G. Preventive analgesia by local anesthetics: the reduction of postoperative pain by peripheral nerve blocks and intravenous drugs. Anesth Analg. 2013;116(5):1141-61. eng. [PubMed ID: 23408672]. [PubMed Central ID: PMC3633654]. https://doi.org/10.1213/ANE.0b013e318277a270.
-
14.
Aveline C, Le Hetet H, Le Roux A, Vautier P, Cognet F, Vinet E, et al. Comparison between ultrasound-guided transversus abdominis plane and conventional ilioinguinal/iliohypogastric nerve blocks for day-case open inguinal hernia repair. Br J Anaesth. 2011;106(3):380-6. eng. [PubMed ID: 21177284]. https://doi.org/10.1093/bja/aeq363.
-
15.
Bærentzen F, Maschmann C, Jensen K, Belhage B, Hensler M, Børglum J. Ultrasound-guided nerve block for inguinal hernia repair: a randomized, controlled, double-blind study. Reg Anesth Pain Med. 2012;37(5):502-7. eng. [PubMed ID: 22705951]. https://doi.org/10.1097/AAP.0b013e31825a3c8a.
-
16.
Bari MS, Haque N, Talukder SA, Chowdhury LH, Islam MA, Zahid MK, et al. Comparison of post operative pain relief between paracetamol and wound infiltration with levobupivacaine in inguinal hernia repair. Mymensingh Med J. 2012;21(3):411-5. eng. [PubMed ID: 22828535].
-
17.
Ko SH, Lim HR, Kim DC, Han YJ, Choe H, Song HS. Magnesium sulfate does not reduce postoperative analgesic requirements. Anesthesiology. 2001;95(3):640-6. eng. [PubMed ID: 11575536]. https://doi.org/10.1097/00000542-200109000-00016.
-
18.
Albrecht E, Kirkham KR, Liu SS, Brull R. Peri-operative intravenous administration of magnesium sulphate and postoperative pain: a meta-analysis. Anaesthesia. 2013;68(1):79-90. eng. [PubMed ID: 23121612]. https://doi.org/10.1111/j.1365-2044.2012.07335.x.
-
19.
Chen Y, Zhang Y, Zhu YL, Fu PL. Efficacy and safety of an intra-operative intra-articular magnesium/ropivacaine injection for pain control following total knee arthroplasty. J Int Med Res. 2012;40(5):2032-40. eng. [PubMed ID: 23206490]. https://doi.org/10.1177/030006051204000548.
-
20.
Dabbagh A, Elyasi H, Razavi SS, Fathi M, Rajaei S. Intravenous magnesium sulfate for post-operative pain in patients undergoing lower limb orthopedic surgery. Acta Anaesthesiol Scand. 2009;53(8):1088-91. eng. [PubMed ID: 19519724]. https://doi.org/10.1111/j.1399-6576.2009.02025.x.
-
21.
De Oliveira GJ, Castro-Alves LJ, Khan JH, McCarthy RJ. Perioperative systemic magnesium to minimize postoperative pain: a meta-analysis of randomized controlled trials. Anesthesiology. 2013;119(1):178-90. eng. [PubMed ID: 23669270]. https://doi.org/10.1097/ALN.0b013e318297630d.
-
22.
Turan A, Memis D, Karamanlioglu B, Guler T, Pamukcu Z. Intravenous regional anesthesia using lidocaine and magnesium. Anesth Analg. 2005;100(4):1189-92. [PubMed ID: 15781543]. https://doi.org/10.1213/01.ANE.0000145062.39112.C5.
-
23.
Narang S, Dali JS, Agarwal M, Garg R. Evaluation of the efficacy of magnesium sulphate as an adjuvant to lignocaine for intravenous regional anaesthesia for upper limb surgery. Anaesth Intensive Care. 2008;36(6):840-4. eng. [PubMed ID: 19115654]. https://doi.org/10.1177/0310057x0803600614.
-
24.
Naderi Nabi B, Sedighinejad A, Haghighi M, Hasanzadh Moghadam H, Ghazanfar Tehran S, Ashoori Saheli N. Evaluating the effect of adding Magnesium sulfate to intrathecal lidocaine on duration of postoperative analgesia in lower limb orthopedic surgeries. JAP. 2014;5(3):20-8. Persian.